EHF Poll Headlines:
Nearly 7 in 10 Texans say they skipped or postponed medical care because of cost
66% of Texans without health insurance say they do not have a primary care doctor
Texans with chronic medical conditions or poor health are more likely to face non-medical issues like unaffordable housing, little access to healthy food, no places to exercise
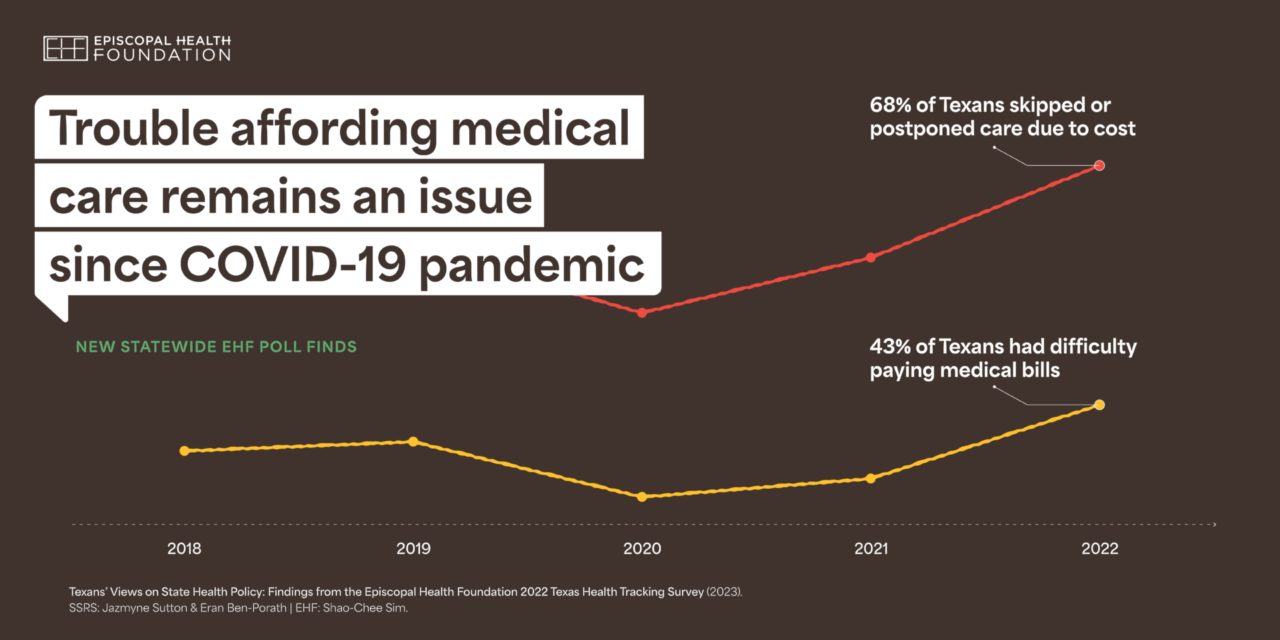
Almost 7 out of 10 Texans say they skipped or postponed medical care in the past year because of cost, including check-ups, treatments, and filling prescriptions. That’s the highest percentage of Texans who say they skipped care in the five-year history of the Episcopal Health Foundation (EHF) annual poll on health care affordability and access in Texas, and just one of the worrying results of the latest statewide survey.
“This is more than a health care crisis; It’s a statewide crisis,” says Dr. Ann Barnes, president and CEO of Episcopal Health Foundation. “These numbers paint a grim picture of the barriers Texans face in accessing essential medical care.”
Overall, the poll shows that 50% of Texans say they put off getting health care they need, 42% skipped a recommended medical test or treatment, and 35% did not get a prescription filled due to the costs.
“When people put off care or skip a treatment they need, it often leads to worsening health and even higher costs down the road,” says Dr. Barnes, a physician who previously oversaw clinic services at several safety-net health systems in Texas. “A recent national study showed that nearly 60% of people who delayed getting care during the pandemic said their existing medical conditions got worse, not better.”
Texans have trouble affording health care, paying medical bills
When Texans did seek health care, the poll shows that more than half of those surveyed (52%) said it’s difficult for them to afford health care. More than two-thirds of low-income Texans (68%) said they had struggles affording medical care compared to just 34% of higher earners. Hispanic (62%) and Black (55%) Texans said they had more trouble affording health care than White (44%) Texans.
EHF’s survey finds that four in 10 Texans (43%) say they had difficulty paying their medical bills. That number is up from 35% last year and it’s the highest percentage of Texans reporting trouble paying medical bills in the five years EHF has conducted the statewide poll.
Many Texans, especially the uninsured, say they don’t have a primary care provider
In addition to affordability issues, EHF’s poll shows that more than a quarter of Texans (28%) say they do not have a primary care doctor or provider that they usually see for regular checkups, when they are sick, or when they need health advice.
Again, for Texans without health insurance the numbers are even more concerning – 66% of uninsured Texans under age 65 do not have a primary care provider. That’s compared to 21% of Texans with health insurance and under age 65 who say they don’t have a primary care doctor.
“Without regular primary care people are missing out on prevention and routine screening, especially for chronic conditions like diabetes and high blood pressure, and even some cancers,” Dr. Barnes says. “That can lead to a delayed diagnosis, severe health complications, ER visits, and missing time at work. The results are much higher costs for Texans and the overall health system.”
EHF’s poll shows that more than 1 in 10 of Texans (13%) do not have a regular place where they receive medical care or rely on hospital emergency rooms. Younger adults (15%), Hispanic Texans (19%), and those with lower income levels (20%) are more likely to say they do not have a usual place where they receive care.
Most Texans say they’ve experienced a non-medical factor impacting their health
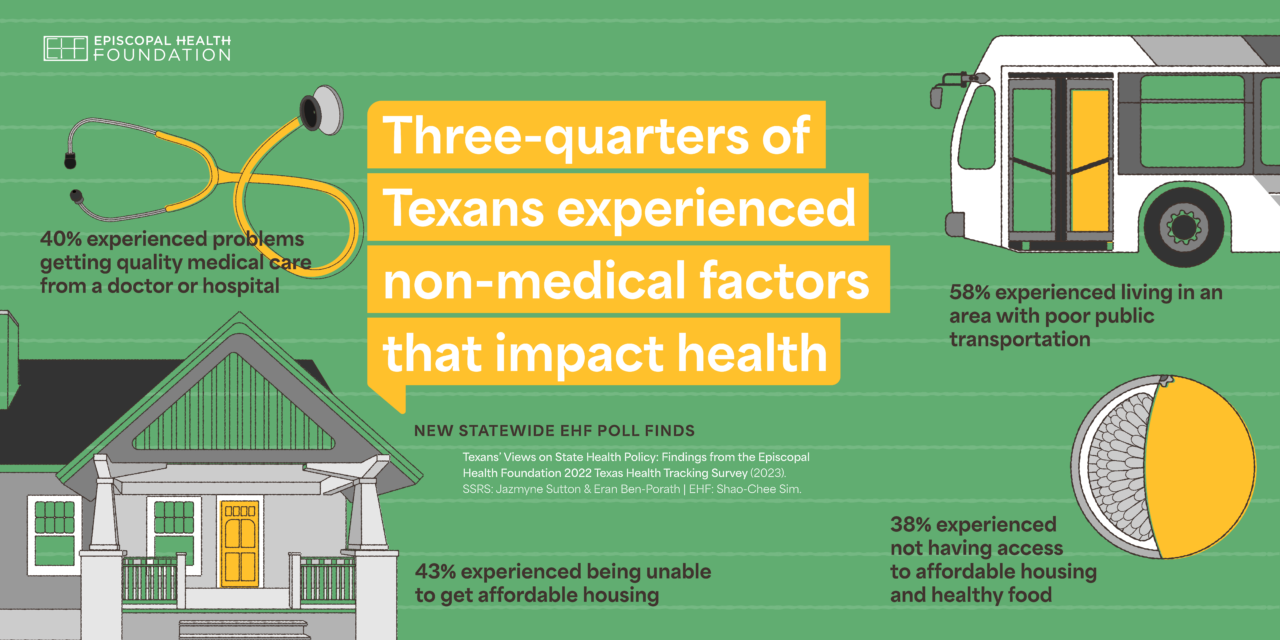
It’s not just problems getting medical care that is affecting the overall health of Texans. The poll finds that 75% of Texans say they experienced a non-medical factor impacting their health.
Those non-medical factors include issues like lack of job security (65%), living in an area with poor public transportation (58%), not being able to get affordable housing (43%), racial or ethnic discrimination (43%), problems getting quality medical care (40%), living in an area without essential resources (40%), or not having access to affordable housing and healthy food (38%).
Texans in poor health or battling chronic medical conditions are more likely to face certain non-medical problems. More than half of Texans (53%) who report they are in poor health said they lacked access to affordable housing and healthy food compared to just 34% of those in good health. Similarly, 41% of those in poor health say they don’t have a place to exercise compared to 28% of Texans in good health.
“These numbers reveal what my patients at safety-net clinics taught me – their health concerns were predictable yet preventable outcomes of the challenging social and economic circumstances they faced,” Barnes said. “True health goes beyond the doctor’s office. We must confront the unequal and unacceptable health realities by addressing the root causes of poor health in communities.”
About two-thirds (65%) say Texans would be healthier if the state spent more money on non-medical factors that affect around 80% of an individual’s overall health outcomes. More than half (55%) say that insurance providers should cover non-medical factors that affect people’s health and 73% say it is very important or essential for doctors to ask about non-medical factors.
“If doctors and clinics ask about non-medical factors and then health insurance plans start to pay for things like food prescriptions and interventions by community health workers, then we’ll begin to get better health outcomes,” Barnes says.
Texans say costs for basic necessities that impact health are rising
Finally, the poll finds that Texans have experienced a sharp decrease in their ability to afford basic necessities as inflation continues to affect household budgets. The poll shows 41% say it’s difficult to afford food, an increase of more than 10 percentage points from 2021 when 29% percent said it was difficult to afford food.
Similarly, 54% say it is difficult to afford gas and other transportation costs in 2022 compared to 42% in 2021.
Methodology
SSRS conducted the latest wave of the Texas Health Policy Survey on behalf of Episcopal Health Foundation from September 27 through October 31, 2022. The goal of this survey was to understand the perspectives and experiences of Texas adults regarding their health care and health care policies in the state, with a comparison to similar studies completed in 2018–2021. The 2022 Texas Health Policy Survey, was conducted online and by telephone with a representative sample of 1,201 Texas adults (age 18 or older). Interviews were administered in English (n=1,102) and Spanish (n=99). The sample includes 601 Texas adults reached through the SSRS Opinion Panel and another 600 reached from a random digit dial telephone sample of landline (n=169) and cell phone (n=431) numbers. The margin of sampling error for this study is +/- 3 percentage points for results based on the total sample.