Texas has the largest rural population in the nation, and the health of rural populations is critical to our state. More than 75% of the counties in the Episcopal Diocese of Texas are considered rural. Yet, many of these rural communities lack basic preventive, primary, behavioral, and oral health services.
If we keep doing what we’ve been doing, then we’ll keep getting the same results. That’s why EHF is dedicated to improving the health of rural communities by approaching health at all angles.
First, EHF’s 2018-2022 Strategic Plan outlines specific objectives to improve rural health, including increasing availability to basic primary care services and strengthening the health system in these communities.
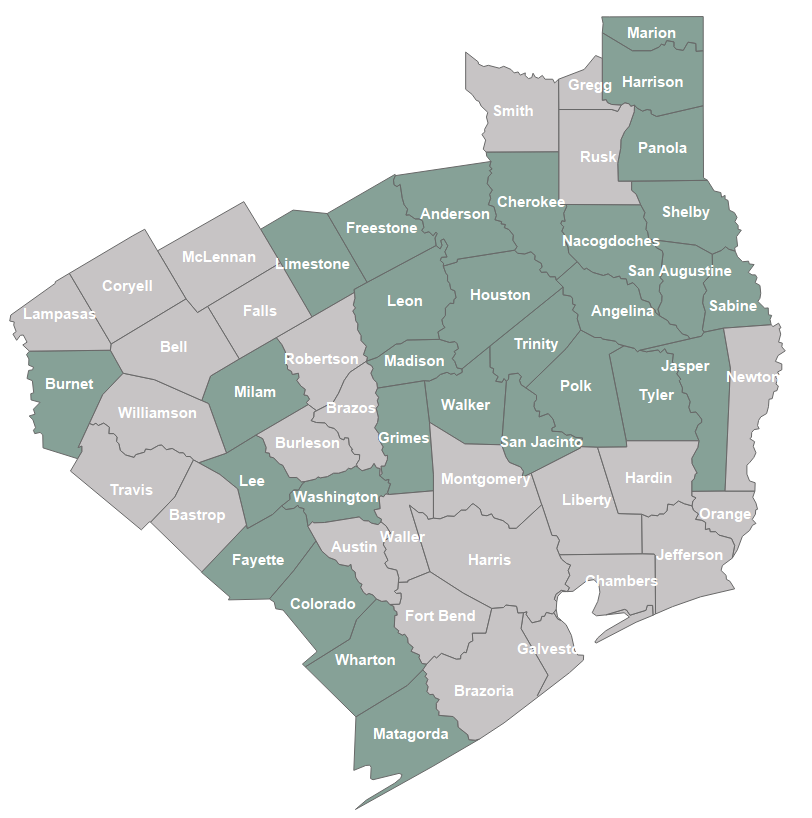
Figure 1. The counties in the EDOT that have been designated as rural by the US Office of Management and Budget are Anderson, Angelina, Burnet, Cherokee, Colorado, Fayette, Freestone, Grimes, Harrison, Houston, Jasper, Lee, Leon, Limestone, Madison, Marion, Matagorda, Milam, Nacogdoches, Panola, Polk, Sabine, San Augustine, San Jacinto, Shelby, Trinity, Tyler, Walker, Washington, and Wharton.
Current research shows that the populations and communities in rural areas face different circumstances and challenges than urban areas. The people who live in rural areas tend to be older, have higher rates of chronic disease, with lower incomes and less access to healthcare. Additionally, the changing health system is bringing unique challenges to rural areas. Many communities depend on rural hospitals whose futures are now in jeopardy.
EHF’s research division’s work on rural health is designed to not only better inform the work of the Foundation, but these rural health reports and resources may also prove useful to congregational members working to improve the health of their communities.
EHF sponsored the Rural Hospital Environmental Impact Study by the Texas Organization of Rural and Community Hospitals (TORCH). The study shows that Texas is bearing the brunt of the rural hospital closure epidemic hitting the rest of the nation. Since 2013, 16 rural hospitals have closed across the state. The study outlines recommendations, taking into consideration state and federal policies and the unpredictable state of the Affordable Care Act.
A separate EHF-sponsored report outlines practical options for Texas communities facing a rural hospital closure. In What’s Next? Practical Suggestions for Rural Communities Facing A Hospital Closure, authors at Texas A&M University’s Rural and Community Health Institute look at alternatives beyond only whether or not to close a hospital. They found that ideas like expanding tele-medicine, converting a former hospital into a freestanding emergency room, or establishing new rural health clinics are some of the many successful healthcare alternatives available to communities at risk of losing a traditional rural hospital.
On EHF’s County Health Data map, you can find county-level data and information about population demographics, health outcomes, access to health, mental health, health behaviors, and social needs for adults and children.
 EHF’s recent research on the impact of Hurricane Harvey also includes rural counties. The study examines 24 of the hardest-hit Texas counties, including three rural counties: Colorado, Matagorda and Walker. EHF’s Harvey project includes an interactive map showing FEMA assistance requests and approvals for every zip code affected by the storm.
EHF’s recent research on the impact of Hurricane Harvey also includes rural counties. The study examines 24 of the hardest-hit Texas counties, including three rural counties: Colorado, Matagorda and Walker. EHF’s Harvey project includes an interactive map showing FEMA assistance requests and approvals for every zip code affected by the storm.
For more information on any of these reports or data, send an email to research@episcopalhealth.org