In addition, two-thirds of Texans say people would be healthier if the state spent more money on non-medical factors that affect health. Those are just some of the results of Episcopal Health Foundation’s first-of-its-kind statewide survey on how government and the health care industry can address social determinants of health in Texas.
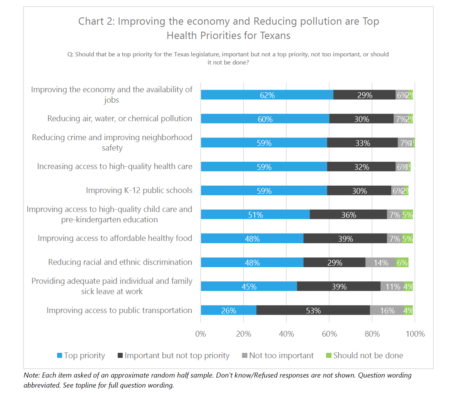
EHF’s survey found that 62% of Texans said that improving the economy and availability of jobs should be a top priority for the state legislature when it comes to improving the health of residents. Similar numbers say that reducing air, water or chemical pollution (60%), reducing crime and improving neighborhood safety (59%), and improving public schools (59%) should also be top state health priorities.
“COVID-19 is clearly showing what Texans already know: the state needs to address underlying, non-medical conditions that have a dramatic impact on their health,” said Elena Marks, EHF’s president and CEO. “Low-income and minority communities are more likely to catch the virus in the first place and more likely to get sicker and die if they do catch it. All of that goes back to social, community, and economic conditions — not medical care.”
EHF’s survey also found that low-income Texans were more likely than those with higher incomes to say that addressing factors like the economy, crime, racial discrimination, and access to child care and Pre-K education should be top health priorities for lawmakers.
In addition to naming various community conditions as health priorities, researchers found that two-thirds of Texans (66%) say that people in Texas would be healthier if the state spent more money on non-medical factors. That’s more than twice as many Texans who said the state shouldn’t invest in those issues (29%). Women, young adults between ages 18-29, and low-income Texans were the groups most likely to say more state spending on non-medical factors leads to a healthier Texas.

“These numbers, along with the disparities highlighted by COVID-19, should spark important discussions by state leaders on how they can address underlying causes of poor health that have nothing to do with going to a doctor or hospital,” said Marks. “So many Texans face a range of social and economic conditions that conspire against their health. We have to change the conversation to improving health, not just health care in Texas.”
EHF’s survey also asked about the role Texans think health insurance companies should play in addressing community factors that impact health. Nearly six in 10 (58%) say health insurance should help cover non-medical factors that might affect people’s health. Researchers found that women, younger adults, non-whites, and those with lower incomes were more likely to say insurance companies should help cover non-medical factors.
This report was released as EHF celebrates five years of actively working to improve community health in Texas. These findings are the second in a series of reports drawing on EHF’s survey of Texans’ views of social determinants of health. In EHF’s first report, researchers found that more than half of Texans (57%) said they think having good medical care is not enough for a person to live a healthy life and that factors like where you live, how much money you make, and how much stress you have are all critical to overall health.
Methodology
SSRS, an independent research company from Glen Mills, PA, conducted the Texans’ Views on Social Determinants of Health Survey on behalf of Episcopal Health Foundation by telephone from October 10 – November 19, 2019 among a random representative sample of 1,200 adults age 18 and older living in the state of Texas. Sampling, data collection, weighting and tabulation were managed by SSRS in close collaboration with Episcopal Health Foundation researchers. The margin of sampling error for this study is plus or minus 4 percentage points for results based on the total sample. For results based on subgroups, the margin of sampling error may be higher.
To schedule an interview, contact Brian Sasser, EHF’s chief communications officer, at bsasser@episcopalhealth.org or 832-795-9404 cell.
