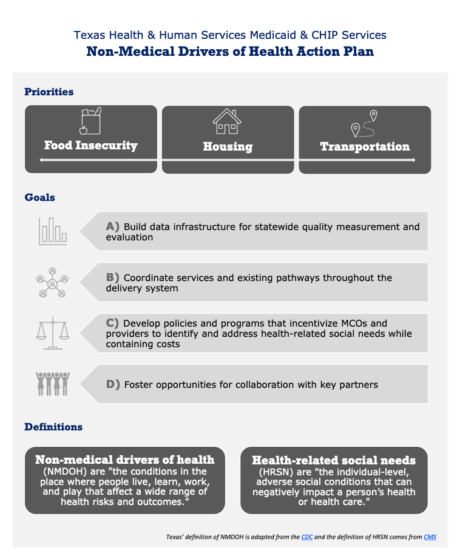
The Texas Health and Human Services Commission (HHSC) has released a new, groundbreaking action plan to address non-medical drivers of health (NMDOH) through Medicaid & CHIP by focusing on food insecurity, housing, and transportation.
NMDOH include various non-medical factors related to the conditions in which people live, work, play, and age that influence their health and wellness.
HHSC’s plan outlines steps and goals for Texas Medicaid and CHIP services to coordinate NMDOH activities through health care providers and the Managed Care Organizations (MCOs) that deliver Medicaid health insurance to low-income Texans. The plan’s goal is to pursue cost savings, reduce use of medical services, and improve health outcomes by going beyond the doctor’s office and dealing with non-medical factors that lead to poor health.
“This is a great step and an extraordinary opportunity to address underlying factors that impact health on a larger scale with sustainable funding across the state,” said Dr. Ann Barnes, EHF’s president and CEO.
After HHSC’s announcement, Barnes and other EHF leaders were in Austin to lead discussions and participate in two important state efforts related to the new NMDOH action plan.
Barnes and and EHF’s Shao Chee Sim first led a presentation at the state’s Value Based Payment and Quality Improvement Advisory Committee outlining how EHF’s grants, research, and community engagement efforts have worked together to reshape the debate about health and health care in Texas.
“EHF’s innovative spirit in improving #HealthNotJustHealthCare is at the forefront of changing the conversation to addressing non-medical root causes of poor health in new and different ways,” Barnes says.
EHF invests resources for research projects that provide evidence of cost savings and health improvements when health insurance programs address non-medical factors that impact health. As a philanthropy, EHF has also funded a variety of clinic and nonprofit projects — including food as medicine and asthma home remediation programs — that have shown great health improvements for patients. But those projects were often pilot programs or other efforts limited to patients of a single clinic or area.
“The new state efforts could be a game changer for Texans most in need,” Barnes said. “It’s changing the way we think about health and how we pay for it.”
In December, EHF released Moving Upstream – an in-depth research report revealing detailed evidence of health improvements and cost savings when Medicaid covers programs that address non-medical factors. Researchers outlined the benefits of project focused on asthma home remediation, food as medicine, and support services for housing programs.
The report is part of the committee’s 2022 legislative recommendations that urge state lawmakers to expand “upstream” Medicaid programs to cover non-medical drivers of health.
In addition to overseeing the Moving Upstream report, EHF’s Sim was appointed to serve on the committee for a two-year term, leads the committee’s NMDOH work group, and also serves as a member of the committee’s Alternative Payment Models work group.


Barnes and Sim also presented updates to the state’s MCO NMDOH Learning Collaborative meeting at the Texas Medical Association in Austin.
EHF has been a key funder and organizer of the collaborative’s effort to help MCOs learn about effective strategies for addressing Medicaid beneficiaries’ non-medical needs. The learning collaborative kicked off in 2019 and brings together Texas MCOs with national and state experts with ideas about best practices, new interventions, important partnerships, and more.
Along with EHF’s presentation, this latest meeting included breakout sessions to get feedback about HHSC’s new action plan from MCOs, health care providers, other stakeholders.